Treatment: Steps To Success
Did you know that gum disease is an infection of the gums...
...rather than simply a lack of care!
Gum disease affects 50% of the adult population and in most cases it is a sign of bacterial and parasite oral infection, as discussed previously. The amoeba Entamoeba gingivalis is the most common micro-organism found in all cases of periodontal diseases. It's presence is easy to confirm by using a Dark Phase Microscope and a video system with which you can view your clinical procedures and results. These parasites are very mobile, they are able to defend themselves against our immune system, they have highly pathogenic characteristics and they also produce "pus" in the gums. They are typically associated with the jaw bone destruction and gum deterioration. Certain general symptoms can appear as we have previously outlined.
Entirely eliminating the parasite Entamoeba gingivalis and pathogenic bacteria leads to rapid and steady recovery of chronic and aggressive periodontitis including stopping the bleeding, eliminating bad breath and closing the infected periodontal pockets: on condition that the residual tartar is carefully removed and that the natural healing of the gum can proceed. A parasite is an organism which lives at the expense of its host. By definition there can be no non-pathogenic parasite. Only the degree of pathogenicity might be questioned.
Signs and symptoms, associated with an infection of the oral cavity by Entamoeba Gingivalis, frequently included apparent difficulty in maintaining a clean mouth, with heavy plaque formation which rapidly regenerated after brushing, or other plaque control procedures; an unpleasant taste, an awareness of the gums, which bleed easily; ulcerations; halitosis (pungently reminiscent of garlic) sore, dry or itchy eyes and a history of generalised malaise, fatigue and frequent headache. Protracted or repetitive 'Flu' like symptoms were often reported if the infection had been recently contracted. Typically, initial infections might be accompanied by little or no transient soreness. Following an asymptomatic period, which may represent an incubation stage, there followed a ‘ flu' like illness which was typically severe or repetitive. Rather than a return to normal health, patients seemed to acclimatize to a diminished state of health with undue fatigue and more frequent headaches.
This phenomenon may indicate a sudden release of virus and/or other antigenic material. Systemic disturbance, which may be loosely described as ‘ Flu’, is sometimes noted following routine dental procedures, particularly "scaling and cleaning".
Since Entamoeba gingivalis is about the same size as white blood cells, on which it feeds, instrumentation around a site infected with protozoa could also produce a parasitaemia. It is not surprising, then, to find similar pathology in rheumatoid arthritis and destructive periodontal disease. A correlation between arthritis and oral amoebiasis has been observed. Over fifty years ago Kofoid reported finding entamoeba in the bone marrow of some arthritic subjects. This would help explain the historical relationship between arthritis and periodontal diseases and a vogue for treating arthritis with anti protozoal drugs. We find, in the treatment of periodontal disease, that following the elimination of Entamoeba Gingivalis, some patients with arthritis report a dramatic reduction in signs and symptoms of the disease. This improvement is usually maintained unless the patient becomes re-infected.
A Modern Microbiological approach by Dr Mark Bonner
International Institute of Periodontology.
The parasites E.gingivalis and possibly its counterpart E. Hystolytica as well as the flagellum Trichomonas tenax found in the mouth act as aggressive pathogens and should be treated as such. Trichomonas tenax has been isolated from tonsillar suppuration and chronic purulent pulmonary disease. This might indicate that it's habitat is the mouth and related structures in the respiratory tree.
Eliminating oral parasites generally prevents the use of traditional surgical procedures which have become futile. Their existence in gum disease is unacceptable and their removal ensures rapid healing as seen by microscopic assessments and clinical exams. E.gingivalis can also be found in infected tonsillar area along with Actinomyces bacteria, producing a white "Cottage cheese" specs.
Entamoeba gingivalis is disregarded by most dentists and parasitologists, regarding this amoeba as a nonpathogenic organism of no importance in the causation of periodontal or other disease. Some even regard this parasite as beneficial and a scavenger of cellular debris and bacteria. Entamoeba gingivalis has been seen to ingest both erythrocytes and leukocytes in addition to the nuclei of leukocytes. Infection with Entamoeba gingivalis might thus be termed a disease in which the patients leukocytes ( White Blood Cells —your immune system) are being consumed by the disease. This is compatible with opinion that Entamoeba gingivalis is pathogenic. Although we would not yet be prepared to state that oral protozoa are present in all cases of ulcero- membraneous gingivitis, (Vincent’s Infection, NUG, ANUG, Erythema Multiforme etc) we have found them to be present in all the cases we have seen. Prolonged elevation of IgM class antibody in recurrent ulcero membraneous gingivitis has been observed by us and reported by Lehner in 1967. This, as he states, would be consistent with a protozoal aetiology for this type of periodontal disease.
Step 1 - Your Clinical Examination & Microbiological Diagnosis
We will provide a diagnosis by using the microscope and clinical signs and symptoms and a thorough oral examination including a whole Jaw xray, and any further testing that is indicated for you. 
Evaluations of tissue damage are supplemented with microscopic assessments of periodontal disease associated microorganisms and the presence of white blood cells (WBC). Complete samplings of periodontal disease associated microorganisms are important to distinguish the “SPECIFIC SITE” nature of the disease process. The infection is very subtle, cunning, and difficult to clear. The GOAL of therapy is to achieve HEALTH. The infection is both inside and outside the body.
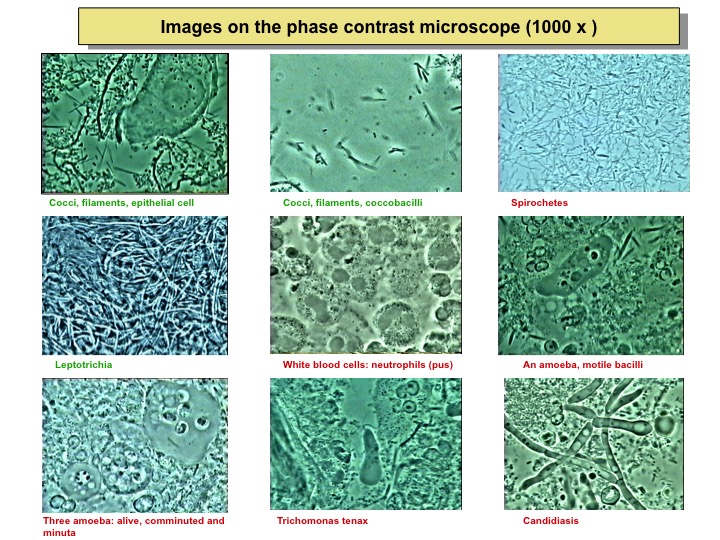
Are you affected? Microscope Results
Healthy - The gums are pink, The rim of the gum adheres to the teeth, No bleeding. Coccoid bacteria; Immobile filamentous bacteria; some epithelial cells.
Gingivitis - The gums bleed easily, Bad breath and a bad taste in the mouth occur. The gums are bluish. Mobile spiral- shaped and snake like Bacteria; spinning Rods.
Early
Periodontitis - The Gums recede, Bleeding is more pronounced. Radiography shows a slight bone deterioration. A 4 mm "pocket" appears around the teeth. White blood cells; Mobile bacteria ; Amoeba parasites present
Moderate
Periodontitis - Gums recede, Abscesses can develop around the teeth. Radiography shows angular bone degeneration. The "pocket" reaches 5 - 6 mm around the teeth. Many white blood cells; Mobile bacteria; Well established parasites
Advanced
Periodontitis - Teeth begin to loosen The "pocket"now reaches 7 +mm , the bone shows significant deterioration. Creation of pus; Mobile bacteria; Nests of parasites
Step 2 - Your Education
You are informed about the nature of periodontal infections, specific bacterial, protozoal, or fungal risk factors, how tissue damage occurs, and the possibility of transmission of organisms from person to person. Developments in research and conceptual approaches in treating THE DISEASE PROCESS are continually being investigated worldwide.
Significant factors are microbial and parasitic 1) Types , 2) Numbers, 3) Activity, and 4) Organizational patterns, as well as 5) White blood cell (WBC) counts.
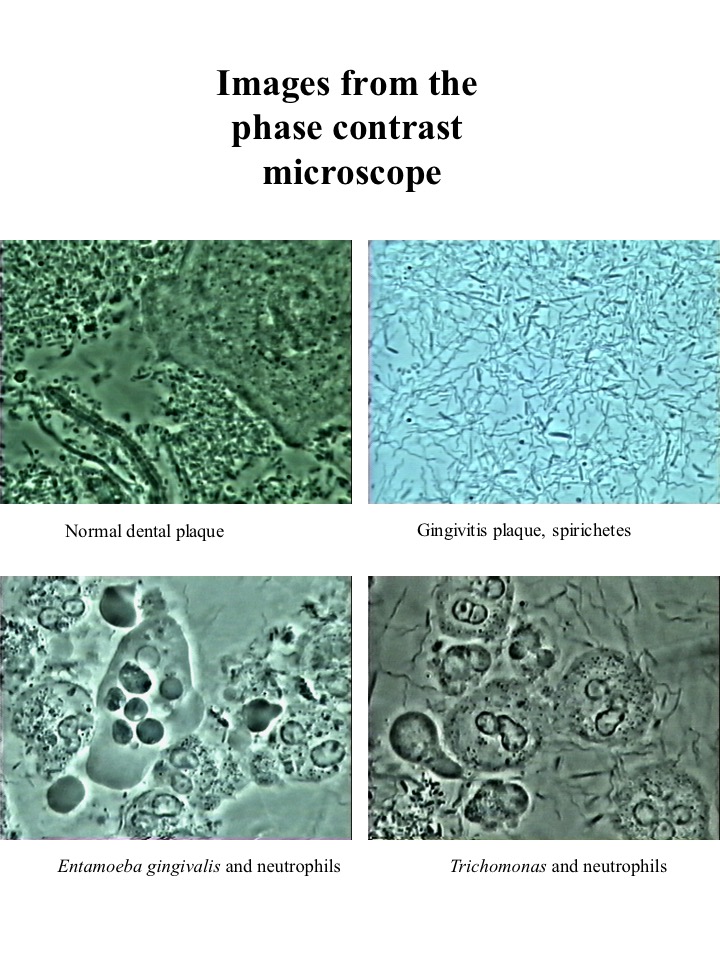
To achieve optimum periodontal health and avoid reinfection, we also aim to identify and eliminate the possible sources of periodontal pathogens. Periodontal Disease Can Be Transmitted To Your Children and Spouse. New DNA coding techniques have allowed researchers to trace the path of infection from one person to another. Periodontal disease was found to be transmitted by saliva contact between family members. Periodontal disease bacteria and parasites travel from the pockets around your teeth into saliva. Transmission of the infection through saliva is influenced by how often a person is exposed to your saliva and their susceptibility to getting the disease. In family settings, saliva contact occurs quite often.
Some common ways that saliva contact occurs between family members are:
- Kissing
- Coughing
- Sneezing
- Sharing food
- Sharing a cup or glass
- Sharing utensils or drinking straws
How did you get the "periodontal disease" in the first place? Most of the time, the answer is “from your parents when you were a child.” It is important not to pass along your infection to your children. Husbands can give periodontal disease to their wives and wives can give it to their husbands.
Pets, such as Old Dogs can also be a source, if your dog licks you. Also Tropical Vacations and contaminated food or water can be a source of the infecting organism. Some re-infections are associated with underlying systemic disorders, particularly blood sugar issues, chronic exposure to environmental pollutants, occupational or familial contacts, &/or a patient's social habits (for example, the sharing of food). But both direct and indirect mouth-to-mouth contact must be considered, as must a number of other factors which contribute to the vulnerability of the individual to become infected. Reinfection is to be expected until patients are prepared to make changes in their lifestyles and habits.
How Can I Help My Family?
First, you must complete all recommended periodontal treatment.
Studies have found that periodontal treatment gets rid of (or greatly reduces) the level of periodontal bacteria in your saliva.
Second, you need to keep your periodontal cleaning appointments. Research has found that, without periodontal cleanings, some bacteria in the saliva can return to pre-treatment levels within six months. They conclude that patients can significantly reduce their risk of re-infection (of themselves and their family members) through frequent periodontal cleanings.
Should I Have My Family Screened?
Screening of spouses or Partners and children is important in many cases, and we look forward to seeing your loved ones. If you have concerns about family members, we suggest you schedule an appointment for them.
If we find indications of periodontal infection we may recommend your family member:
- Do additional oral hygiene at home.
- Have more frequent dental cleanings.
- Receive periodontal treatment
Why Is Transmission Of Periodontal Disease Serious?
Periodontal infection is responsible for 75% of all adult tooth loss. Lost teeth must be replaced with dental work which can be both expensive and less natural looking.
Periodontal infection has also shown to increase the risk of Heart Disease, Heart Attack and Stroke, Fertility issues, Arthritis and a host of other systemic health concerns. Beyond the scope of what has already been generally accepted about periodontitis (such as its connection to cardiovascular disease and rheumatoid arthritis, recent studies continue to offer new, additional information that suggests disease in the gums can spread to other parts of the body and/or disease in other parts of the body can impact the gums.
A 2000 study by Li, Kolltveit, Tronstad, and Olsen published in Clinical Microbiology Reviews entitled “Systemic Diseases Caused by Oral Infection” examined the links between periodontal disease and cardiovascular disease, infective endocarditis, bacterial pneumonia, low birth weight, and diabetes mellitus. The researchers of this study specified that bacteria from the mouth could be passed to the bloodstream: With normal oral health and dental care, only small numbers of mostly facultative bacterial species gain access to the bloodstream. However, with poor oral hygiene, the numbers of bacteria colonizing the teeth, especially supragingivally, could increase 2- to 10-fold and thus possibly introduce more bacteria into tissue and the bloodstream, leading to an increase in the prevalence and magnitude of bacteremia. Other researchers have explored the association between oral infection and illness as well.
To eliminate the external sources of infection, wash your hands after handling your pets.
Encourage your partner to get assessed for pathogens to avoid transmission from one to another.
A personalised Total Body Health program can also be designed by Nutrition Diagnostics to correct the imbalances of your general health that may be impacting your oral health.
- Primarily correcting prediabetes, diabetes or metabolic disease which is underpinned by too many carbohydrates, and a poor protein and iron status. ( minerals of Oxidation )
- Controlling smoking, consumption of sugar and caffeine which facilitates the growth of pathogenic flora.
- Local factors that may delay or prevent the proper course of treatment are defective restorations, infected root canals, heavy metals (mercury) amalgams, poorly fitting fixtures & appliances. These factors need to be addressed and treated under safe guidelines.
Step 3- Patient Instruction
You are instructed in an effective self-care program using INSTRUMENTS and AGENTS that combat periodontal disease associated microorganisms.
Using antiseptics ( The Brushing Solution & PerioMix) and
antibiotics where appropriate and necessary, we eliminate the Bad Bugs.
This phase may take several months and will be punctuated with monthly microbiological sampling to assess the progress of your flora and
adjust your treatment.
You will receive Home Care instructions and treatment that works and is validated by measurement of the improvements not only clinically but
microscopically.
COMPLIANCE in homecare is an absolute must in attaining and maintaining control of the periodontal disease associated
microorganisms and END POINTS of therapy.
Step 4- Professional Treatment
Treatment includes meticulous debridement of root surfaces (1-10 hours) and irrigations with antiseptic AGENTS to the depths of all pockets. Piezoelectric ultrasonic units have recently been adapted for subgingival instrumentation and are proving to be excellent additions to the periodontal armamentarium. The infection is treated prior any scaling and removal of Calculus or tartar subgingivally.
For the first time in dentistry quality of homecare and professional treatment is MEASUREABLE by using a Dark Phase Microscope. The word clean mouth now has a new definition, and the therapist and patient know “THE THERAPEUTIC END POINT” is reached.
Step 5 - Monitoring and Measuring
After an appropriate interval the patient’s progress is assessed by monitoring for microorganisms and the prevalence of white blood
cells (WBC). Complete and repeated localized monitoring is essential in establishing the END POINTS of treatment as well as assessing the
corroborating clinical signs and symptoms of oral and periodontal health. (pockets, bleeding, colour, pain, shape, odour). In this way
“false negative” readings are held to a minimum. Use of multiple agents is an essential in controlling these mixed infections.
If disease related microbial complexes have not been converted to ones associated with health, and if white blood cell levels remain high,
in- office treatments and home-care programmes need to be modulated. Additional agents should be considered. Systemic antibiotics are
usually necessary to “clear the infection” from the body and COMPLIANCE is very important. Antibiotics will not “clear the
infection” outside the body.
Step 7 - Maintenance-- measuring and monitoring.
The frequency of maintenance or recall visits will depend on such factors as: your age, immune system response, diet, smoking, general health, COMPLIANCE with homecare, dexterity, chances of reinfection, the extent of prior tissue damage, and other variables. The length of time between visits will be influenced by the levels of control attained by both professional and self-care measures after initial therapy.
Those patients that have undergone Total Dental RevisionTM appear to have the best outcome as they have diligently worked with their Health Coach at Nutrition Diagnostics to rebuild their inate immune system.
What to expect ?... with correct treatment and application
Biofilm Before treatment.
Typical biofilm in chronic periodontal disease before Antiparasitic / anti-infective treatment according to Dr Bonner. Microscopic images show many PMNs, amoeba parasites and motile bacteria. When infection is gone, then calculus removal can be done with sonic or ultrasonic instruments. No curettes which would remove cement needed for re-attachment. Compare after treatment healthy commensal biofilm! Periodontal disease is easily detectable, preventable and curable using biofilm microscopic analysis. Stop debridement, stop curettage, stop surfacage, stop surgery! Start removing parasites and leucocytes, than remove calculus gently with piezzos. Cicatrisation is obligatory!
Biofilm After treatment.
Typical biofilm in "cured" chronic periodontal disease after Antiparasitic/ anti-infective treatment according to Dr Bonner/ Lyons Technique. Microscopic images show complete absence of PMNs, parasites and motile bacteria. Only epithelial cells are present, non motile cocoid and filamentous commensal bacteria. Clear bubbles are air bubles in saliva mount as there is a lot less plaque to observe, patient being compliant. Compare with before treatment chronic active periodontitis biofilm!
This patient is now cured! Stress, smoking and genes are not eloquent parameters in periodontal disease and produce no power to cure periodontitis. On the other end, good oral hygiene, parasite removal and white cell elimination renders periodontitis easy to heal! Periodontal disease is easily detectable, preventable and curable using biofilm microscopic analysis.
