The Oral–Gut–Immune Axis: Why Systemic Health Begins in the Mouth
The oral–gut–immune axis is an emerging area of research that reveals how oral health is deeply connected to gut function, immune regulation, and chronic disease development.
Understanding this axis is essential for anyone serious about treating the root causes of inflammation, autoimmunity, or chronic metabolic conditions.
What Is the Oral–Gut Axis?
The oral–gut axis describes the biological and microbial connection between the mouth and the gastrointestinal tract. With every swallow, the mouth seeds the gut with bacteria, viruses, fungi, and even parasites — not occasionally, but trillions of microbes daily.
More than 700 microbial species colonize the oral cavity, including:
- Anaerobes like Porphyromonas gingivalis, Fusobacterium nucleatum, Treponema denticola
- Protozoan parasites like Entamoeba gingivalis and Trichomonas tenax
- Spirochetes and vibrios that are highly motile, invasive, and capable of immune evasion
- Gastric pathogens like Helicobacter pylori, often originating in the mouth before colonizing the stomach
In a healthy person, these organisms are kept in balance. In the presence of oral dysbiosis — from gum disease, root canal infections, or cavitations — they become a constant upstream source of inflammation.
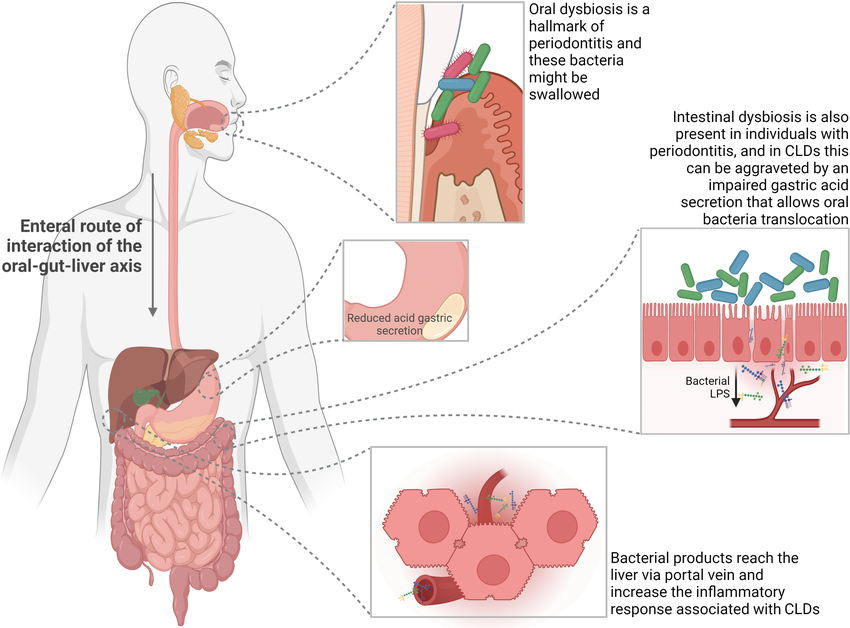
How Oral Pathogens Disrupt the Gut and Beyond
1. Microbial Translocation and Gut Dysbiosis
Pathogens like P. gingivalis and F. nucleatum resist digestion and embed in the gut lining, where they:
- Displace beneficial flora
- Stimulate inflammation
- Alter mucosal barrier function
F. nucleatum in particular has been linked to colorectal cancer, due to its ability to promote tumor microenvironments.
2. Gut Barrier Breakdown
Pathogens from the mouth — including spirochetes and vibrios — can compromise the gut lining, leading to:
- Leaky gut syndrome
- Activation of GALT (gut-associated lymphoid tissue)
- Elevated systemic cytokine production
These changes lay the foundation for autoimmunity, food sensitivities, and chronic fatigue.
3. Immune System Disruption
The immune system is constantly sampling microbial information from the mouth and gut. Oral pathogens generate immune confusion through:
- Molecular mimicry, where bacterial proteins resemble host tissue
- Endotoxemia, especially from lipopolysaccharides (LPS) in gram-negative bacteria
- Chronic low-grade inflammation, leading to immune exhaustion
The Oral–Immune Axis: Immune Dysfunction Starts in the Mouth
The mouth isn’t just a mechanical or digestive gateway. It is a functional immune organ.
- Salivary glands produce IgA, a frontline antibody that neutralizes pathogens before they reach the gut.
- Periodontal tissue houses immune cells, constantly reacting to oral microbiota.
- In cases of gingivitis, periodontitis, or infected root canals, cytokines and bacteria leak directly into the bloodstream, bypassing the gut entirely.
This is the oral–immune axis in action: a pathway through which oral health influences systemic immunity directly — not just via the gut, but via circulating immune messengers.
The Role of Spirochetes, Vibrios, and Oral Parasites
These stealth pathogens are frequently overlooked in standard dental care and even in many functional medicine programs.
- Spirochetes (e.g., Treponema denticola) have been linked to Alzheimer’s, cardiovascular disease, and periodontal destruction. Their corkscrew motion allows deep tissue penetration.
- Vibrios and motile anaerobes create polymicrobial biofilms that are resistant to antibiotics and immune clearance.
- Protozoa like E. gingivalis are found in cavitations, root canal-treated teeth, and periodontal pockets — acting as reservoirs of inflammation.
These organisms can persist for decades unless surgically or energetically addressed. Their chronic presence can sabotage the immune system’s regulatory function and prime the body for systemic illness.
Clinical Implications: Chronic Disease, Cancer, and Autoimmunity
- P. gingivalis and T. denticola secrete enzymes that degrade collagen, immunoglobulins, and cytokines — creating local tissue destruction and systemic immune modulation.
- F. nucleatum has been found in both oral and colorectal tumors, acting as a microbial bridge between the mouth and cancer progression.
- H. pylori originating from the oral cavity may play a role in gastric cancers and autoimmune gastritis.
- Hidradenitis suppurativa, an inflammatory skin condition, may also be fueled by chronic immune dysregulation linked to oral stealth pathogens, particularly when conventional antibiotics fail.
Health Model Thinking: The Mouth as the Starting Point for True Healing
From a Health Model Thinking perspective, the oral–gut–immune axis reinforces one critical truth: If the body is fighting
persistent infections in the mouth, it cannot repair, regulate, or detoxify efficiently.
In our model:
- We do not treat isolated symptoms
- We identify and remove persistent immune insults (e.g., infected root canals, cavitations, dysbiosis)
- We rebuild immune competence through oral detoxification, body chemistry balance, and ancestral nutrition
What This Means for Patients and Practitioners
For Patients:
- Bleeding gums and dental work are not just local issues. They could be fuelling systemic disease.
- You cannot out-supplement or out-diet a chronic oral infection.
- Ask your healthcare team: Has anyone checked my oral–immune status?
For Practitioners:
- Treat the mouth as an immunological organ, not just a mechanical structure.
- Use bacterial DNA, microscopy, or immunological markers to assess oral infection burden.
- Integrate oral detoxification into chronic disease protocols — especially for unresolved inflammation, skin disorders, gut issues, and autoimmune disease.
Final Word
The immune system is the body's central defence and repair network. When it functions well, it orchestrates healing, maintains tolerance, and resists disease. When dysregulated, it drives the progression of nearly every chronic illness known today, from cardiovascular disease to cancer.
Thus, the oral–gut–immune axis are fundamental regulators of health and vitality. They highlight that oral health is inseparable from gut health and immune function, exerting wide-reaching effects on systemic well-being.
The oral-gut-immune axis reinforces a simple but radical idea: Systemic health starts in the mouth.
